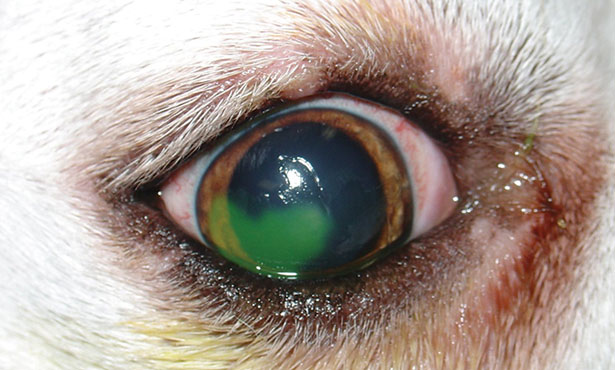
Disorders Associated with Chronic Corneal Ulceration
Refractory ulcers typically result from an unresolved underlying etiology. A thorough history, physical examination, and ocular examination must be performed to exclude possible causes of delayed healing before treatment choices are made. Common disorders associated with refractory corneal ulceration include adnexal disease such as entropion or ectopic cilia, corneal exposure such as with exophthalmos, facial nerve paralysis, or abnormal eyelid conformation, keratoconjunctivitis sicca (KCS), corneal edema due to endothelial degeneration or dystrophy, and corneal accumulation of lipid or mineral.
In middle-aged to older patients (typically 8 years or older), indolent ulceration and spontaneous chronic corneal epithelial defect (SCCED) are the most common reasons superficial ulcers fail to heal. Boxers and golden retrievers are more commonly affected than other breeds. No matter the cause of the initial ulcer, SCCEDs fail to resolve due to abnormal corneal healing from lack of adhesion of the epithelium to the underlying stroma. This is due not only to a deficiency in adhesion molecules but also to development of acellular material within the ulcer bed that physically blocks new epithelial cells from attaching.
[...]
Treatment of SCCEDs
Middle-aged to older dogs with SCCEDs require corneal debridement in addition to the recommendations above in order to achieve healing. You must be certain of your diagnosis before attempting a corneal debridement, which can cause a deep ulcer to perforate or drive infection deeper into the cornea if performed inappropriately. Consult with an ophthalmologist if you have any questions. Corneal debridement can be performed on the awake patient with the help of an experienced assistant to provide head and body restraint or under sedation, whichever is your preference.
The cornea should be gently rinsed and disinfected with 1:20 up to 1:50 dilute betadine solution before applying topical anesthetic. Mechanical debridement with a sterile, dry cotton-tip applicator is performed next, applying mild pressure in sweeping or circular motions targeting the ulcer bed, edges, and adjacent cornea to remove any nonadhered epithelium. The ulcer often becomes a few millimeters larger in this stage, which is important to determine the true extent of abnormal tissue. Once the cotton tip applicator becomes moist, it often loses friction with the cornea and should be discarded. Repeat the process, utilizing a new dry sterile swab as necessary until no further tissue can be removed. Subsequently, a grid keratotomy or diamond burr debridement can be performed, making sure to treat the entire ulcer bed as well as 1 to 2 mm past the edge of the ulcer. Recent studies describing diamond burr debridement and grid keratotomy report a >90 percent healing rate in 10 to 15 days following a single treatment. Punctate keratotomy has fallen out of favor among ophthalmologists due to the development of safer alternatives, such as the diamond burr. It is important to avoid contacting the eyelids or third eyelid with your needle or burr tip. If contact occurs, use a new needle or burr tip to avoid seeding bacteria into the freshly debrided cornea.
Corneal ulceration can occur for a variety of reasons. Ulcers that persist beyond 5 to 7 days despite therapy are considered refractory.

vetmed.illinois.edu